Health & Wellbeing, Maternity
Coping with pelvic instability in pregnancy (pelvic girdle pain)
Coping with pelvic instability in pregnancy (pelvic girdle pain)
Coping with pelvic instability in pregnancy can be very challenging. The true incidence of pelvic girdle pain, or pelvic instability, in pregnancy is hard to determine. Some studies say it affects around 20-50% of pregnancies and at times it can be misdiagnosed, misunderstood or mismanaged.
What is Pelvic Instability?
Pelvic instability is a term, often used interchangeably with ‘pelvic girdle pain’, that is used to group a number of conditions that cause pelvic pain during pregnancy.
The group of conditions covering pelvic girdle pain include:
- Pelvic Instability
- Pubic symphysitis, pubic symphysis dysfunction, Diastasis of the Symphysis Pubis (DSP)
- Symphysis pubis dysfunction (SPD)
- Pelvic Joint Syndrome
- Physiological Pelvic Girdle Relaxation
- Symptom Giving Pelvic Girdle Relaxation
- Posterior Pelvic Pain
- Pelvic Arthropathy
- Inferior Pubic Shear/ Superior Pubic Shear / Symphyseal Shear
Symphysiolysis - Osteitis pubis (usually postpartum)
- Sacroiliitis
- One-sided Sacroiliac Syndrome /Double Sided Sacroiliac Syndrome
- Hypermobility
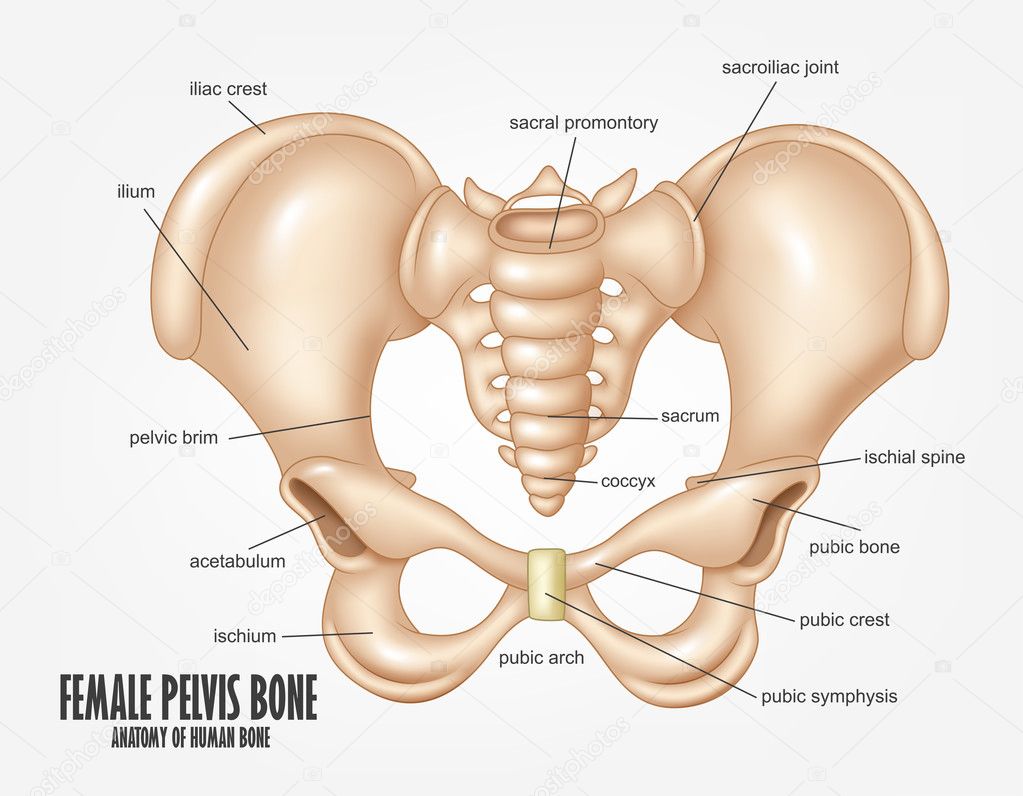
Diagram outlining the bones of the pelvis to show which area relates to different pelvic girdle pain
Why does pelvic pain occur?
Pelvic pain in pregnancy can be caused for a number of reasons including:
- the additional pressure on the pelvis due to the growing baby,
- ligaments softening due to the hormonal changes, or
- changes to your posture.
With all these changes occurring, the pelvis become less stable and can begin to move unevenly. Inflammation can occur, which in turn, will lead to discomfort, pain or even mobility issues.

Pregnant mum holding her back due to pelvic girdle pain
What you might feel
The most common way pelvic instability is felt is in the lower back, over the sacroiliac joints and in one or both hips.
Others may feel pain in the buttocks, down the back of the leg, the groin and inner thigh.
Some women may feel clicking, locking or grinding in their pelvic joints.
Symptoms can occur at any time, but most often develop around 5 months of pregnancy.
It can become more severe as the pregnancy progresses and may start earlier in subsequent pregnancies.
What activities can increase the pelvic pain?
There are a number of activities that can increase pelvic pain. These include:
- Extended periods of walking
- Fast walking
- Going up or downs stairs
- Getting in and out of bed
- Getting in and out the car
- Rolling over in bed
- Lying flat
- Exercises such as running, jumping, squats, lunges
- Standing on one leg
- Moving from sitting to standing

SupaCore Pregnancy Support Shorts
Managing pain caused by pelvic instability
There are ways that you can manage pelvic instability to try and reduce the pain.
- Physiotherapy – visit a physio to get advice on activities you should and shouldn’t do. A physio can also provide you with suitable exercise to assist you to relieve your muscles
- Modified activities – you may find a way to modify your normal activities so you can continue to do them without causing pain
- Avoid heavy lifting
- Reduce the amount of walking that you do
- Rest between activities
- Keep your knees together when getting out of a car or bed or turning over in bed.
- Pain medication – paracetamol is approved for use in pregnancy, however you should consult your doctor when using pain medications to treat any form of pain
- Use a cold pack on the area for 10-20 minutes every 2-3 hours to help reduce inflammation
- Be conscious of good posture at all time and keep your back straight and tall
- Wear a compression garment or support belt. Support belts can be supplied by a physiotherapist or you can try something a bit more comfortable like Supercore Prenatal Compression Shorts.
- Massage to relieve the tight muscles.
Pregnant woman with pelvic instability using crutches
When will the pain go away?
For most women, the pain will go away within a few weeks of delivery. It is important to continue to look after yourself immediately following the birth.
Some tips for managing pelvic instability after birth include:
- Rest lying down when you can
- Continue to wear postnatal compression garments to support your pelvis
- Continue to use cold packs on the affected area
- Don’t overdo it and remember to rest if your pain increases.
Seek medical advice
If you are experiencing pelvic pain during or post pregnancy always consult your doctor and/or physiotherapist who can provide a thorough diagnosis and management and recovery program for you.